No schools, no blood: How Covid-19 closure has worsened shortage
Written by BY GILLIAN NANTUME – September 7th, Daily Monitor, Uganda
Reproductive Health Uganda through the SET SRHR project is advocating for increased funding to the National blood bank.
This is through a campaign dabbed Saving lives through greater investment in safe blood transfusion services.
Join the conversation on social media using #SupportTheUGBloodBank #SaveLives #WeAreRHU
Blood transfusions are a strong pillar in modern medicine and they have saved the lives of countless people. Women with pregnancy related complications need donated blood more than all other groups, except children below the age of five. Dr Elizabeth Nabiwemba, the project director of SET-SRHR, says blood loss mainly affects women in childbirth because their blood levels are already low due to the pregnancy.
Who is at risk
“Haemorrhage is the number one killer of pregnant women. When there is no blood in a hospital the risk of a woman dying in labour is very high. She does not have to lose much blood to die.”
Sarah Mutegombwa, the programme manager for blood donor recruitment at Uganda Red Cross Society (URCS) says most of the donated blood goes to children below five years.
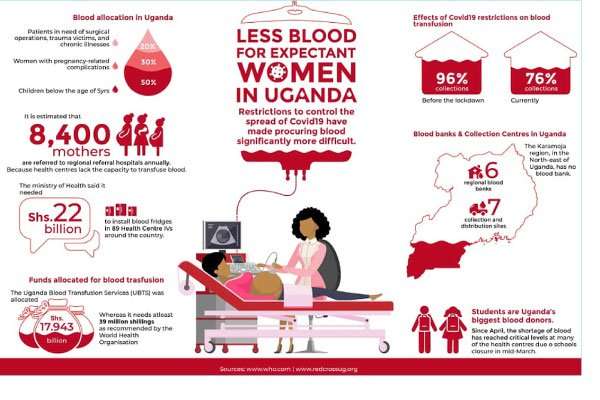
“These children take at least 50 percent of the blood because they become anaemic when they suffer from severe malaria and malnutrition. Women with pregnancy-related complications take up 30 percent of the demand, while the remaining 20 percent is shared by those in need of surgical operations, trauma victims, and those who suffer from chronic illnesses, such as cancer and sickle cell disease.”
Mutegombwa adds that one unit of blood can serve three children, because they use only one or two components of the blood, such as red blood cells, platelets, or the plasma. An adult, though, can consume as many whole units of blood as the need arises. In contrast, in high-income countries about 76 percent of the donated blood is received by patient groups over the age of 65.
Before the COVID-19 pandemic dominated the focus of health policymakers, the Ministry of Health (MoH) had, in its 2020/21 budget, said it would target equipping Level IV Health Centres to provide blood transfusion services in order to improve reproductive, maternal, neonatal, child and adolescent health services.
According to the Health Ministerial Policy Statement for the Financial Year 2020/2021, it is estimated that 8,400 mothers are referred to regional referral hospitals annually because Level IV Health Centres lack the capacity to perform obstetric care as they cannot transfuse blood. The ministry said it needed Shs2.2 Bn to install blood fridges in 89 Level IV Health Centres around the country.
Chronic blood shortages worsened
There are seven blood collection and distribution sites located in the districts of Lira, Nebbi, Jinja, Masaka, Kampala, and Hoima. The collections sites are not fully-fledged blood banks because they do not have testing facilities. Restrictions to control the spread of the coronavirus have made procuring blood, even from these few points, significantly more difficult.
While anyone between 17- 60 years can donate blood as long as they are in good health, students are Uganda’s biggest blood donors.
“During the school term, we run continuous blood donation mobilisations to replenish what is in the blood banks, until the students get holidays. As a country, we have been getting 70 percent of our total blood donations from schools. The remaining 30 per cent is collected from the community. Some areas organise and then, call us, with the intention of donating blood,” Mutegombwa says.
She adds that one nurse could tend to two donors at the same time previously, but due to Covid-19 regulations, a nurse now spends about 15 minutes bleeding one donor.
Who has been donating?
With the broader lockdown came bans on public gatherings and public and private transport. URCS switched to soliciting for blood from individual registered donors.
Uganda has between 80,000 and 90,000 registered blood donors, most of who donate twice a year. Mutegombwa says they would pick donors from home, take them to donation centres, and drive them back.
On average, they picked between 20 to 30 donors per day. Each donor can only donate one unit every three months for males and every four months for females.
Cost of blood supply
The government meets the costs of blood donation. During lockdown, organisations such as the Indian Association offered to transport blood donors.
Although transport resumed later, blood donations remained low due to restrictions on gatherings and continued school closures.
Doctors across Uganda began fundraising initiatives to support blood collection efforts.
The WHO standard
According to the World Health Organisation’s Global Database on Blood Safety, a country should collect blood equivalent to one percent of its population annually.
Uganda’s estimated population requires about 459,035 units of blood annually, but the country’s target remains about 300,000 units.
Coronavirus restrictions worsened collection levels, dropping national blood collection significantly.
Charting a way forward
Efforts are ongoing to mobilise communities, register donors, and encourage voluntary blood donation through outreach, partnerships, and digital tools such as donor-registration apps.
Health officials continue to emphasise that blood donation saves lives and community participation is essential to addressing shortages.






